
Retinal microvascular function assessments provide instant integrated and dynamic data analysis that is specific to each individual. These tests can, however, be complex and time‐consuming, and are performed only in highly specialized services, this contributing to the lack of inclusion of this parameter in the more largely circulated risk scores. Nevertheless, parameters such as retinal microvascular function has been found to show a good association not only with various circulatory markers for CVD 13, 14, but also with other modifiable and non-modifiable risk factors for this disease such as obesity 15, family history 16 and age 17, 18. Assessing vascular endothelial function is usually performed using techniques such as ultrasound flow‐mediated dilation (FMD), pulse wave analysis (PWA), plethysmography and iontophoresis 12. In addition, vascular endothelial function, a parameter often overlooked, is essential not only for investigations into the pathophysiology of CVD but also for better CVD risk stratification 9, 10, 11. Consequently, it has been suggested that other factors, such as obesity, psychosocial stress and lifestyle, to name just a few, should also be included for more precise estimations 8. Indeed, it has been shown that they could either over‐ or underestimate actual risk for CVD in a large number cases 4, 6, 7. These calculations are based, however, only on few non-modifiable as well as some modifiable risk factors, thus limiting their ability to accurately predict the risk for CVD in all individuals. Other risk scores, such as the Prospective Cardiovascular Mὒnster (PROCAM) and the European Society of Cardiology Systematic Coronary Risk Evaluation (SCORE) 4, 5 are also being used for the same purpose. In this way, positive progress is made towards considering individual over population factors when considering someone of being at risk for CVD.īut what is the real measure of a high CVD risk? Today, the gold standard for absolute CVD risk is based on the Framingham 10-year CVD risk score (FRS) 3.
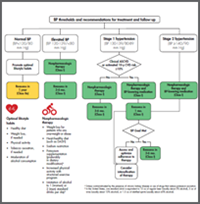
Indeed, both ECC/ESH guidelines and ACC/AHA have recognised this fact and recommended considering treating patients with high CVD risk at a BP threshold lower than their current cut-off for grade/stage 1 HTN 2. Nevertheless, it would seem sensible that, in individuals with higher risk for cardiovascular disease (CVD), early diagnosis and interventions are applied at lower BP values. In addition, such change in practice has also a significant impact on the patients’ physical and psychological wellbeing 1. By using the ACC/AHA guidelines, the number of patients diagnosed with having this disease increased significantly and so did the pressure on the health system and economy.
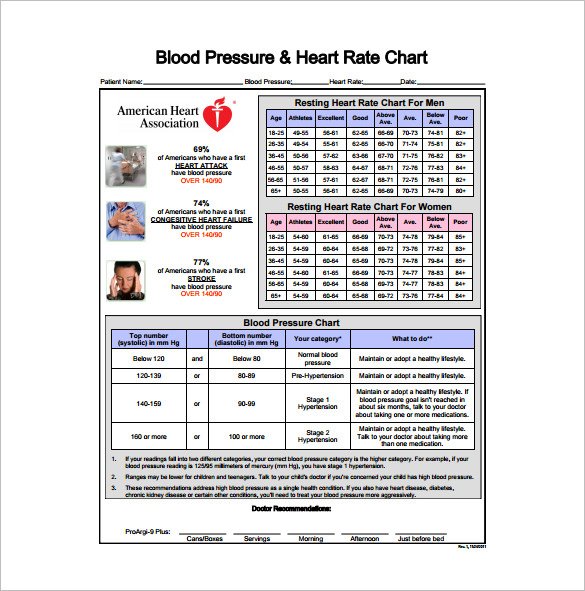

As it can be expected, such difference is bound to have a high impact on clinical diagnosis and management of HTN. One of the main differences between the latest guidelines published in 2018 by the European Society of Cardiology/European Society of Hypertension (ESC/ESH) and those published in 2017 by The American College of Cardiology/American Heart Association (ACC/AHA) is the cut-off for what is considered elevated blood pressure (BP) and the first stage of hypertension (HTN) diagnosis 1. This observation could be important when deciding personalised care in individuals with early hypertensive changes. The conclusion of this study is that microvascular dysfunctions is present at multiple levels only in individuals with ESC/ESH grade 1 hypertension. Peripheral vascular reactivity (aTR) was lower in ESC /ESH grade I compared to those graded ACC/ASH stage I hypertension ( p = 0.0122). In addition, they also had significant lower artery baseline, artery BDF, MD and MC than individuals classed as stage 1 hypertension based on the ACC/ASH guidelines ( p = 0.00022, p = 0.0179, p = 0.0409 and p = 0.0329 respectively). Individuals classed as grade 1 hypertension according to the ESC/ESH guidelines, however, exhibited a significantly decreased artery baseline ( p = 0.0004) and MC ( p = 0.040), higher slope AD ( p = 0.0018) and decreased vein MC ( p = 0.0446) compared to age matched normal individuals. Retinal vascular function measured in all groups belonging to the ACC/ASH classifications were within the normal values for age-matched normal population. Blood pressure and lipid panel were also evaluated. Retinal and peripheral microvascular function was assessed in 358 participants by means of dynamic retinal vessel analysis and digital thermal monitoring, respectively. The aim of this study was to investigate retinal and peripheral microvascular function in asymptomatic individuals that fall into different BP groups when using either the ESC/ESH or the ACC/AHA guidelines.

